Message from Meet the Need NC
Change in our North Carolina Intellectual and Developmental Disabilities (I/DD) Community is fierce. It is a shift to a managed care model for Medicaid coupled with the slow realization of Federal Olmstead legislation. Both of these are dependent on the negotiations between the NC General Assembly House and Senate over the state budget.
How can a person with I/DD or one’s family keep up with all the change? How can we, as an I/DD Community, go forward together with a common goal, without being seen as divided by legislators and other policymakers, and each other for that matter, when we all have such individualized needs?
Whether advocating for more Innovations Waiver slots or Direct Support Professional (DSP) pay increases or deciding whether living/working in the community is your best choice, we all have a common thread that weaves us together. Much of our lives is about navigating systems – and waiting for services and supports. Meet the Need NC has heard countless stories of unmet I/DD service and support needs from those in North Carolina over the last two years. We are all tired of waiting. As an I/DD Community, we want choices from a broad array of services and supports for ourselves and our loved ones based on our individual needs.
We need to transform the way we band together. Driving perceptions around our I/DD Community is bigger than all of us individually. Changing attitudes inside and outside our I/DD Community takes time and requires intention. We must come together around a new narrative where we break out of our own I/DD Community to advocate and inform legislators, teachers, family members, and so many more about the dignity and value of our I/DD Community. Together, we have the best chance to make changes for better, more fulfilled lives, and for our I/DD Community to be more integrated into society.
In this May newsletter, Meet the Need NC provides follow up materials from our May webinar to extend learning about the NC Medicaid Innovations Waiver and DSP caregiver workforce crisis. Additional articles include policy updates, a blog article about the need for the legislature to understand the dire needs of people with I/DD, and highlighted resources and events.
We look forward to having you join us for our June Lunch & Learn where we will focus on the Registry of Unmet Needs (also known as the RUN or Innovations Waiver waitlist). Click here to register.
Please enjoy our May newsletter. And let’s keep climbing the same mountain together!
May Lunch & Learn Wrap Up
Thank you to Corye Dunn, Disability Rights NC and Talley Wells, NCCDD for presenting basic information on the Innovations Waiver and Direct Support Professionals (DSP) / Caregiver Workforce Crisis. Please see the May Lunch & Learn recording, slides, answers to questions not answered during our webinar, and additional resources about the topics below.
Speakers Presentations and Resources
- Video recording of the May 2023 Meet the Need NC Lunch & Learn
- Direct Support Professional Update May 2023 Talley Wells – NCCDD
- Q&A from Webinar about Innovations Waiver
- Q&A from Webinar about Direct Support Professionals
- Q&A from Other Topics
Additional Resources about the Innovations Waiver
- Am I Eligible for an Innovations Waiver? (Disability Rights NC)
- NC Innovations Waiver (NC Medicaid)
- HCBS: Home and Community-Based Services: Programs to Support Community Living – DRNC (Disability Rights NC)
- LME/MCO Directory – Find your LME/MCO. Call to ask about applying for Innovations Waiver or verify they have your current information.
Additional Resources about Direct Support Professionals (DSPs)
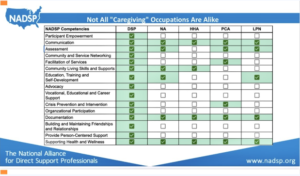
Source: From NADSP Advocacy Symposium: Amplifying the Voices of DSPs, May 3-4, 2023 presentation
- DSPs help support those with I/DD daily. DSPs help people become integrated and engaged in their community. They aim to assist people in realizing their full potential. (National Alliance for Direct Support Professionals)
- What is a Direct Support Professional (DSP) and the importance of DSPs to community-based living (Office of Disability Employment Policy)
- Programs to Support Community Living (Disability Rights NC)
- A Day in the life of a Direct Support Professional (video from the Autism Society of NC)
Register for the June Lunch & Learn!

We meet on the third Tuesday of every month at noon with new topics brought to you by thought leaders in the I/DD community.
Throughout our series, Meet The Need NC intends to create a basic understanding of the unmet needs of those living with I/DD in North Carolina. You can register for one or all of our lunch and learns on Hear. Share. Act: A Lunch & Learn Disability Advocacy Series.
Our next Lunch & Learn will be on June 20 from noon – 1PM. The topic is The Registry of Unmet Needs: The Waiting List for the NC Innovations Waiver presented by Jenna Flynn, Integrated Care Professional with the North Carolina Autism Society.
Click Here to Register!
LENS: Lived Experience Network Speaks
Meet the Need NC is including a blog article in its monthly newsletter, sharing opinions of individuals from our LENS (Lived Experience Network Speaks) advisory group. Our LENS advisory group includes individuals with I/DD lived experience — people with I/DD and their families/caregivers. We provide a space to share freely but these opinions do not necessarily represent all those of Meet the Need NC advisory group members.
“To be candid, there is no substitute for money”

Those are the words of North Carolina Labor Commissioner Josh Dobson during a news conference at the Legislative Building in Raleigh last week. Commissioner Dobson, in addition to representatives from four state agencies and one member of the NC House of Representatives, were discussing the need for higher raises for state employees to combat the problem of “the growing vacancy rate among state employees.” Meanwhile, state and local governments tout the recruitment of companies relocating to North Carolina and the influx of high paying jobs. However, employers, the State included, are unable to fill crucial positions across North Carolina.
Representative Donna White is quoted as saying “We are in a mess” and Ardis Watkins, Executive Director of the State Employees Association of North Carolina, stated “We’ve got issues that are going to lead to tragedy.”
These are dire situations that require the attention and action of members of the NC Legislature working on the State’s budget. However, there are other dire situations that unfortunately do not get this kind of attention and action from our State leaders. Currently, 17,008 North Carolinians with Intellectual and Developmental Disabilities (I/DD) are waiting for Home and Community-Based Services (HCBS) through the NC Innovations Waiver (Waiver). The Waiver waitlist is called the Registry of Unmet Needs (RUN). At the same time, a good portion of the 14,386 people with I/DD who receive the Waiver are not getting the support they need because of the Direct Support Professional (DSP) workforce crisis. Meaning, those fortunate to have the Waiver are also not being served because of the lack of qualified DSPs to fill the thousands of positions the Waiver would potentially employ.
Several bills filed in both the NC House and NC Senate that start to alleviate these crises for those with I/DD have been stalled and sitting in legislative committees for months. Alternatives to these bills have been added to the proposed House Budget Bill and the Senate Budget Bill. However, instead of proposing serious solutions that will have a positive impact on the lives of people with I/DD, the House has included funding for 250 Waiver slots and the Senate has included funding for 350 Waiver slots while 17,008 people wait on the Registry of Unmet Needs. Both budget bills include a $6.50 per hour increase for DSPs. This increase might make a difference if the average rate for DSPs was not so meager.
There is the argument that funding more Waiver slots is premature given the DSP workforce crisis. Let’s get out of this bureaucratic cycle and do both. It is possible and practical to fund more Waiver slots and provide benefits to the recipients. Not all the supports and services provided by the Waiver require DSPs. Why make so many people live with these extremely serious situations when the solution is obvious and the right and moral thing to do?
Cathy Truitt, Superintendent of Public Instruction, said “A meaningful investment in the state’s workforce now – both for state employees and teachers – would produce tangible benefits for decades to come.” This is true of the return on investment and the boost to the North Carolina economy that would be realized by funding a significant number of Waiver slots and increasing the hourly pay rate for DSPs to be competitive among other industries. Members of the NC Legislature need to fix this mess and avoid tragedy by prioritizing people with I/DD just as they are considering solutions to the vacancy rate among State employees. There is no substitute for money.
For more information about this crisis, read an article from the News and Observer (May 25, 2023).
About the author: Donna Beckmann has been involved in the Down syndrome community since the birth of her son in November 2000. She is the Advocacy and Outreach Director for the North Carolina Down Syndrome Alliance working on local, state and national initiatives benefiting people with Down syndrome and other Intellectual and Developmental Disabilities. Donna has established relationships across the disability spectrum and across agencies and organizations in North Carolina. She was the driving force in the creation of Down syndrome specific web pages for the North Carolina Department of Health and Human Service’s website. In addition to a degree in Political Science, Donna has completed North Carolina’s Partners in Policymaking and was a Fellow at the Carolina Institute for Developmental Disabilities LEND – Leadership Education in Neurodevelopmental Disorders Program.
Public Policy Update
Policy updates as of May 24, 2023
These policy updates provide recent updates with rules, bills and other initiatives that relate to services and supports for people with I/DD. While we don’t lobby, we do want you to stay informed, and support having an engaged community who can share how these proposed changes will impact their lives personally.
Innovations Waiver
Summary of Innovations Waiver Slots Legislation Filed to Date
| HB259, Section 9E.10. (House Budget bill) | Proposed Senate Committee Substitute for HB259, Section 9E.10. (Senate Budget bill) | SB566 Increased Innovations Waiver Slots (primary sponsor Sen. Grafstein, DRNC attorney) | |
| Bill Status | House passed its budget and sent it to the Senate | Senate released its budget on 5/15 | Passed First Reading and Referred to Senate Rules; no movement since 4/5. |
| Number of Slots | 250 one time | 350 one time | 2,000 per year for two years (4,000 total) |
| Deadline for implementation | 7/1/2023 | 7/1/2023 | First 2,000 by 10/1/2023 |
| Appropriation | $6.1M Year1 and Year2 | $10M Year1 and Year2 | $36.7M Year 1 and $72.5M Year2 |
| Other | Would repeal Section 9F.14. of S.L. 2021-180 (Appropriations Act) that appropriated $10M recurring for, Group Home Stabilization and Transition Initiative. | Slot allocation based on current policy and would condition additional slots by region on MLE/MCO network adequacy and DSP wages of $18/hr. |
Summary Of Innovations Waiver DSP Wage Increase Legislation Filed to Date
| HB440/SB488 Direct Care Work Wage Increases/Innovations Waiver | HB259, Section 9E.15. (House Budget bill) | Proposed Senate Committee Substitute for HB259, Section 9E.15. (Senate Budget bill) | SB550 Direct Support Professional Wage Increases (primary sponsor Sen. Grafstein, DRNC attorney) | |
| Bill Status | Passed First Reading and referred to House Appropriations Committee; no movement since 3/23 | House passed its budget and sent it to the Senate | Senate released its budget on 5/15 | Passed First Reading and Referred to Senate Rules; no movement since 4/5. |
| Wage Increase | $6.50/hr. increase effective when enacted | $6.50/hr. increase effective when enacted | $6.50/hr. increase effective when CMS-approved | $3.25/hr. increase Year1, then $3.25/hr. Year2 |
| Appropriation | $90M Year1 and Year2 | $60M Year 1 and Year2 | $60M Year1 and Year2 | $72M Year1 and Year2 |
| Funding Mechanism | Directed payment to LME/MCOs; increased LME/MCO rate payment to provider agencies with mandatory 75% going to DSP wages. | Directed payment to LME/MMCOs; increased rate payment from LME/MCOs to provider agencies with mandatory 85% going to DSP wages. | Increased PMPM to LME/MCOs; increased LME/MCO rate payment to provider agencies; provider rate increases eligible for DSP wages or DSP benefits or payroll expenses (no threshold % going to DSP wages). | DHB may recoup if provider audit doesn’t show full 90% going to DSPs. |
| Other | SHB shall recoup if provider audit doesn’t show full 75% going to DSPs = mandatory COLA rate methodology SPA | DHB shall recoup if provider audit doesn’t show full 85% going to DSPs. | DHB shall recoup part or all of the funds…if provider audit doesn’t show use of the increased funding to”to the benefit of” its Innovations DSPs. | DHB may recoup if provider audit doesn’t show full 90% going to DSPs. |
NOTE: Due to the related [April] Centers for Medicare and Medicaid proposed rule (see summary quote below), the NCGA may be in ‘watch and wait’ mode on whether CMS will require an 80% passthrough of provider reimbursement rates to DSP wages. So, we’ll keep an eye on that!
- “For HCBS, we propose to establish additional transparency and interested party engagement requirements for setting Medicaid rates for HCBS, alongside a proposed requirement that at least 80% of Medicaid payments for personal care, homemaker, and home health aide services be spent on compensation for direct care workers (as opposed to administrative overhead or profit).”
- See CMS Press Release and Proposed Rule summary here.
Competitive Integrated Employment (CIE)
Kenneth Bausell, in his new role as Senior Director of Employment at the Division of Vocational Rehabilitation (soon to be called the Office of Employment and Inclusion if the renaming legislation is enacted), recently shared the Division’s top policy priorities:
- Employment First, one of the Governor’s mandates
- Transition to Community Living
- Competitive Integrated Employment
- Olmstead Plan
Please see the most current NC DMH/DD/SAS & DHB Joint Communication Bulletin on CIE and the related Memorandum of Agreement between Disability Rights North Carolina, the Center for Public Representation, and NC DHHS.
Appendix K Flexibilities
Reminder: the federal Public Health Emergency ended on May 11, 2023. The Appendix K Flexibilities for the TBI, Innovations, CAP/C, and CAP/DA will remain in place for an additional six months. They will therefore expire on November 11, 2023.
- Deb Goda, Associate Director of Behavioral Health and I/DD in the Division of Health Benefits, recently reported that the Innovations Waiver amendment to be effective 10/1/2023 will include Appendix K flexibilities that DHHS wants to make permanent before the November 11, 2023 expiration date. Those permanent flexibilities will include but not be limited to:
a) home delivered meals;
b) day supports once a week won’t be required;
c) telehealth will continue to be authorized when appropriate for the beneficiary;
d) direct care services may be provided in alternative settings;
e) parents of minor beneficiaries will be eligible to provide community supports (higher SIS levels only will be approved by CMS – higher level meaning qualifies for Innovations);
f) community navigator only available under Innovations; and more.
DHB will be posting the amended waiver soon for public comment; a Waiver renewal is also coming up soon too, so changes not made for the 10/1 amendment can also potentially be addressed via the renewal.
1915(i) State Plan Option
There are numerous Medicaid Clinical Coverage Policies posted for notice & comment, including new 1915(i) State Plan Option policies (the 8H ones). You can use the quick links below to view the posted policies. Submit comments for policies listed below open for public comment by emailing: public.comment@dhhs.nc.gov.
| Proposed Policy | Date Posted | Comment Period Ends |
| 8H-6, Community Transition (*New Policy) | 04/10/2023 | 05/25/2023 |
| 1K-7, Prior Approval for Imaging Services (Termination) | 05/11/2023 | 06/11/2023 |
| 8N, Intellectual and Developmental Disabilities Targeted Case Management (Termination) | 05/11/2023 | 06/26/2023 |
| 8H-4, Respite (New Policy) | 05/19/2023 | 07/03/2023 |
| 8H-3, Individual and Transitional Support (New Policy) | 05/19/2023 | 06/03/2023 |
- Individuals who have an open 1915(b)(3) service authorization and will enroll in a Tailored Plan will transition to 1915(i) services by Oct. 1, 2023. This means that to transitions their 1915(b)(3) service authorization to 1915(i), they must have complketed a 1915(i) assessment and have a Care Plan/ISP in place that meets 1915(i) requirements by Oct. 1, 2023 (see additional detail below).
- Individuals who have an open 1915(b)(3) service authorization and will remain enrolled in NC Medicaid Direct when Tailored Plans will transition to 1915(i) services by July 1, 2024. This means that to transition their 1915(b)(3) service authorization to 1915(i), they must have completed a 1915O8) assessment and have a Care Plan/ISP in place that meets 1915(i) requirements by July 1, 2024 (see additional detail below). For the purpose of phase-in, LME-MCOs should target completing the 1915(i) independent assessment in the individual’s birthday month.
Read the full fact sheet: North Carolina’s Transition of 1915(b)(3) Benefits to 1915(i).
I/DD Legislative Priorities for North Carolina Organizations
Many organizations decide to focus on advocating by educating and informing on issues. Some of their resources can be referenced below.
NCCDD (North Carolina Council on Developmental Disabilities)
- 2023 Public Policy Priorities
- Policy education meetings every second Thursday of the month from 10:30am-12:00pm via Zoom
The Arc of NC
- Legislative Agenda 2022-23
- Weekly Wrap-Ups with Executive Director, John Nash
Disability Rights NC
Autism Society of NC
The Coalition
Did you know?
In 2015, the NC General Assembly enacted legislation directing North Carolina Department of Health and Human Services (DHHS) to transition Medicaid from fee-for-service to managed care.
Under managed care, the state contracts with insurance companies, and Managed Care Organizations (MCOs) which are paid a predetermined set rate per enrolled person, called the Per Member/Per Month or PMPM rate. Learn more about North Carolina’s Transformation to Medicaid Managed Care.
Olmstead was based on the Americans with Disabilities Act (ADA). Olmstead says people with disabilities have the right to live in the community. It says that people do not have to live or receive services in an institution, nursing home, or any other setting separated from others without disabilities to get the services they need. Those services should also be provided in the community. To learn more about the Olmstead Plan, read What Is North Carolina’s Olmstead Plan?
The NC General Assembly House of Representatives and Senate are currently in the process of negotiating a State budget which includes a spending plan for two years. The House and Senate have separately passed proposed budgets, and now they are deliberating to come up with a one, compromise budget. This is a good time for you to share your stories with your legislators about issues that are important to you. To find your legislators, go to How to Find and Contact your Legislator to tell your story.
Highlighted Resources and Events
- Spring i2i Center for Integrative Health conference, Raleigh, June 12-14, 2023: LAND/MHTA’s panel presentation “Changing the I/DD LANDscape in North Carolina” is on June 12th at noon about the Meet the Need NC initiative which is using a collective impact model. Find out more here.
- How to Find and Contact your Legislator to Tell Your Story: Put your address into this form and it will provide you with the email and telephone numbers of the General Assembly legislators (House and Senate) who represent the county where you live.
- How to apply for Innovations Waiver or Check Up on Your RUN (Registry of Unmet Needs or waitlist) Status:
- Sign Up: If you or a family member have an I/DD, contact your Local Management Entity-Manage Care Organization (LME-MCO) and request the NC Innovations Waiver. If you are found to be eligible, you will be put on the RUN (Registry of Unmet Needs or waitlist). Ask about the availability of alternative services while you wait.
- Use the interactive map or list to find your LME-MCO organization by clicking on the LME/MCO Directory.
- Sign Up: If you or a family member have a diagnosed or undiagnosed I/DD and you do not have Medicaid for income or disability, contact Medicaid to make an application: How to Apply for NC Medicaid | NC Medicaid (ncdhhs.gov).
Visit our Statewide Resources web page for more resources!
Stay in touch with us!
- Register for our email list: Sign up here
- Follow us on social: Facebook & Instagram
- Subscribe to our YouTube channel to view our Lunch & Learn presentations
- Listen to our podcast: The Waiting Room hosted by Kenneth Kelty
